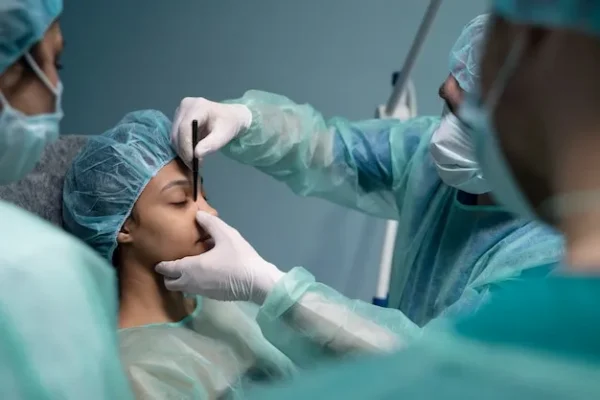
Whether you’re managing a private cosmetic clinic or supporting hospital-based reconstructive procedures, accurate billing isn’t just about getting paid—it’s about protecting your revenue, maintaining compliance, and giving your patients a seamless financial experience.
We’ve worked with plastic surgeons, practice managers, and RCM teams across the country to streamline billing processes, reduce denials, and boost collections. And here’s what we know: plastic surgery billing is different.
From distinguishing between cosmetic and medically necessary procedures to applying the correct CPT codes and modifiers, this specialty requires precision at every step.
At Cadence Collaborative, we understand how complex medical billing and coding can get, especially in the world of plastic surgery.
In this guide, we’ll walk you through everything you need to know—from the basics to advanced coding strategies. We’ll break down codes, give you documentation tips, and share what really works in the real world.
What Is Plastic Surgery Billing?
Plastic surgery billing is the process of converting surgical services into billable claims—either to insurance payers or directly to patients—using standardized codes and compliant documentation.
In this field, accuracy is non-negotiable. Why? Because billing errors can lead to claim denials, delays in reimbursement, or worse, compliance audits.
We divide billing into two primary categories:
- Reconstructive procedures – These are often medically necessary and covered by insurance (e.g., post-mastectomy breast reconstruction, cleft palate repair).
- Cosmetic procedures – These are elective, typically not covered by insurance, and billed directly to patients (e.g., liposuction, facelift).
At Cadence Collaborative, we help plastic surgery practices establish a clear billing workflow for both scenarios. That means proper patient intake, payer policy checks, and code selection from day one.
What Is RCM in Plastic Surgery?
Revenue Cycle Management (RCM) is the end-to-end process of tracking and managing patient revenue, from the first appointment to the final payment.
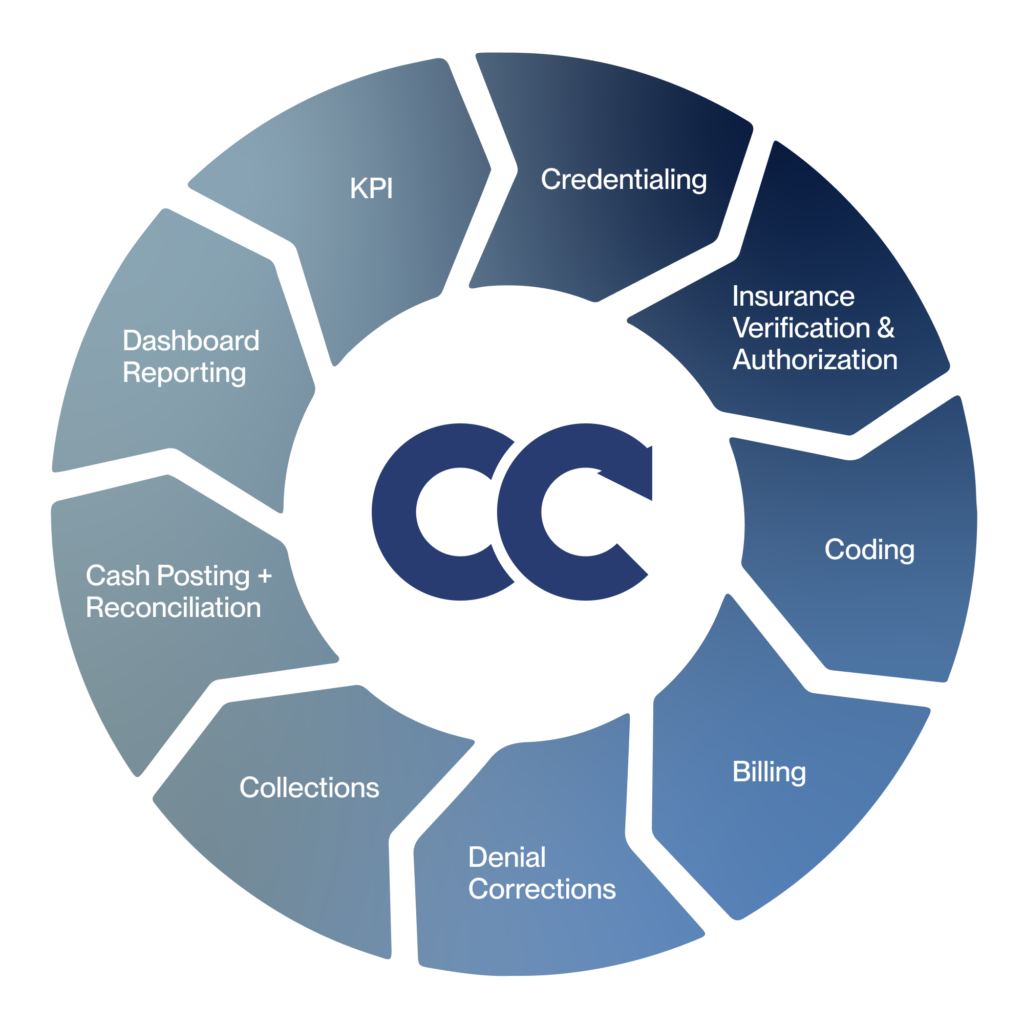
In plastic surgery, where billing may involve both insurance and direct-pay models, revenue cycle management needs to be extra adaptable and proactive.
At Cadence Collaborative, we view RCM not just as billing, but as a growth engine for your practice.
How Plastic Surgery Billing Works (The Real Process)
A strong billing system is more than codes and claims—it’s a workflow that connects your front desk, clinical staff, coders, and RCM team. When those handoffs break down, so does your cash flow.
Here’s the ideal plastic surgery billing workflow we help practices implement:
Step-by-Step Billing Workflow
- Pre-Visit
- Patient registers
- Insurance eligibility confirmed
- Financial counseling for hybrid or cosmetic services
- Prior authorization submitted (if needed)
- Patient registers
- Day of Procedure
- Surgeon documents detailed operative note
- Clinical photos and consent forms are attached to chart
- Surgeon documents detailed operative note
- Post-Op Billing
- Charges entered within 24 hours
- CPT/ICD-10 codes assigned by certified coders
- Modifiers and global period flags added
- Charges entered within 24 hours
- Claim Submission
- Claims scrubbed and sent to payers
- Self-pay invoices sent to patients (with payment links/options)
- Claims scrubbed and sent to payers
- Follow-Up
- Rejected/denied claims corrected within 7–10 days: Working with Cadence, rejected and denied claims are actively addressed as soon as they’re received. Our dedicated team works daily on resolving these denials and rejections, aiming for full resolution within 7–10 days.
- Underpayments appealed
- Outstanding balances are monitored weekly
- Reporting & Review
- Monthly reviews of KPIs: Days in AR, Denial Rate, Collection Rate
- Ongoing training for staff and surgeons on documentation trends
- Monthly reviews of KPIs: Days in AR, Denial Rate, Collection Rate
Cadence Approach: We plug into your existing systems or bring our own tools to manage the entire billing lifecycle, ensuring nothing slips through the cracks.
How to Code for Plastic Surgery
Coding in plastic surgery relies heavily on Current Procedural Terminology codes, ICD-10 diagnosis codes, and the correct modifiers to tell the full story of each procedure.
Let’s look at a few core examples that come up in both cosmetic and reconstructive contexts:
Common CPT Codes
| Procedure | CPT Code | Use Case |
| Blepharoplasty (upper eyelid) | 15822 | Covered if ptosis impairs vision |
| Abdominoplasty | 15847 | Cosmetic unless linked to hernia repair |
| Breast reconstruction (TRAM flap) | 19367 | After a mastectomy, often covered |
| Liposuction, 1 area | 15876 | Cosmetic, direct pay |
| Scar revision (simple) | 13100 | Functional or cosmetic, varies |
| Tissue expander removal | 11970 | Often used post-mastectomy |
Tip from Cadence: Always document why a procedure is being performed. A good medical necessity narrative is the difference between approval and denial.
Modifiers You’ll Use Often
| Modifier | Meaning | Why It Matters |
| -59 | Distinct procedural service | For unbundling services |
| -22 | Increased complexity | When the surgery is more extensive than usual |
| -GY | Non-covered service | Use for cosmetic services billed to insurance |
| -51 | Multiple procedures | If several surgeries are performed together |
What About ICD-10?
Diagnosis codes matter just as much as procedure codes. They justify the medical need behind a surgery, and determine whether a claim is payable or denied.
Here are some plastic surgery ICD-10 examples:
| Condition | ICD-10 Code |
| Dermatochalasis (excess eyelid skin) | H02.83 |
| Congenital breast asymmetry | Q83.8 |
| Post-mastectomy status | Z90.13 |
| Nasal airway obstruction | J34.89 |
| Keloid scarring | L91.0 |
Cadence Tip: Always align ICD-10 codes with the operative report and progress notes. If the documentation doesn’t match, the claim won’t stand a chance.
How to Improve Collections in Plastic Surgery
Plastic surgery practices face a unique challenge: mixed payer models. While reconstructive surgeries may involve commercial or government payers, cosmetic procedures are typically self-pay. This creates operational complexities that demand strategic RCM (Revenue Cycle Management) practices.
At Cadence Collaborative, we help plastic surgeons build resilient, profitable billing systems by aligning front-end workflows, coding accuracy, and payment capture.
Here’s how to boost your collections—without sacrificing patient experience.
1. Set Clear Financial Expectations
For cosmetic procedures, clear and upfront communication is essential. Patients must clearly understand:
- What is included in the fee (pre-operative care, anesthesia, follow-up appointments).
- What is excluded from the fee (complications, revisions, additional facility costs).
- Your payment terms (initial deposit, balance due, available financing options).
Clearly outline the importance of:
- Running eligibility and obtaining prior authorization: This helps provide the patient with accurate expectations regarding their financial responsibility, including determining any potential insurance coverage.
- Collecting a deposit: Secure a deposit to confirm patient commitment and cover initial administrative costs.
- Collecting the remaining balance prior to surgery: Ensuring full payment before the procedure protects the practice from potential revenue loss, as chasing payments post-service can be significantly more challenging.
2. Require Pre-Payment for Cosmetic Procedures
This is standard in the industry. We recommend:
- 10–20% deposit at consultation
- Balance due 7–10 days before surgery
Leverage digital payments, e-signatures, and integrations with software like Square, CareCredit, or HintMD to modernize the experience.
3. Bill Reconstructive Services Promptly & Accurately
If you’re performing reconstructive procedures (e.g., Mohs closures, breast reconstruction, post-trauma repairs), you need to:
- Submit claims within 24–48 hours of documentation
- Use correct CPT and ICD-10 pairings with strong medical necessity
- Attach photos, LMNs, pathology, and progress notes as required
4. Use Financial Counseling for Hybrid Cases
Many procedures fall into a “medically necessary with cosmetic elements” gray area:
- Septorhinoplasty (30420)
- Breast reduction with lift (19318 + 19316)
- Scar revision (13100)
Offer pre-surgical counseling to explain what’s covered vs. out-of-pocket. This builds trust and reduces billing surprises.
5. Implement Real-Time Eligibility Checks
Before the patient arrives for surgery, verify:
- Active insurance coverage
- Authorization requirements
- Copay and deductible estimates
- Policy exclusions (e.g., cosmetic clauses)
We recommend using integrated tools with your PM/EHR system or outsourcing this to Cadence Collaborative’s pre-cert team.
6. Track Your Denials—Then Eliminate Them
Top reasons for plastic surgery claim denials include:
| Denial Reason | Fix |
| Lack of prior auth | Build pre-cert checklists per CPT |
| Missing documentation | Require photo uploads, LMNs, and surgeon letters |
| Bundled procedures | Apply modifiers (-59, -51) and review NCCI edits |
| Non-covered cosmetic claims sent to payer | Flag cosmetic CPTs with modifier -GY or bill directly |
Use denial tracking dashboards or work with us at Cadence to audit trends monthly. You can’t fix what you don’t measure.
7. Offer Financing Options
Plastic surgery is expensive—even medically necessary procedures can result in high deductibles. Offer flexible payment options like:
- In-house payment plans with autopay
- 3rd-party financing (CareCredit, Alphaeon)
- Buy-now-pay-later (BNPL) platforms
Advanced Coding Strategies
When it comes to coding for plastic surgery, the basics won’t cut it.
Multi-procedure cases, complex reconstructions, and hybrid cosmetic-medical surgeries require advanced strategies that go beyond assigning a CPT and moving on.
Combine Procedures the Smart Way
Performing multiple procedures in one session? You need to know how to sequence them and apply the right modifiers.
For example:
Case: Patient undergoes panniculectomy (15830) and hernia repair (49560)
- These procedures are often bundled
- To get both paid, use modifier -59 on the less-valued code
- Include op report notes detailing distinct operative fields
Cadence Note: Always check NCCI edits (National Correct Coding Initiative) to confirm if procedures are bundled. If so, modifier -59 or -XS is essential to “unbundle.”
Use Modifier -22 When Workload Is Significant
Modifier -22 (increased procedural services) should be used strategically.
For example:
Case: Revision of prior abdominoplasty complicated by extensive adhesions, mesh removal, and reconstruction
- CPT: 15847
- Modifier: -22
- Attach a detailed operative report and a cover letter outlining:
- Why the work exceeded usual complexity
- Estimated extra time (e.g., 90 minutes longer than usual)
- Surgical risks, complications
- Why the work exceeded usual complexity
We help clients pre-emptively build modifier-22 justification templates—this reduces rejections and delays.
Know When to Use -51 vs. -59
Modifier -51 is used for multiple procedures that are not bundled, while -59 is used to unbundle when edits exist.
Example:
- Z-plasty (CPT 14040)
- Scar excision (CPT 11442)
- Use -51 on the second code if no edits exist
- Use -59 if they are typically bundled
Quick rule:
- Use -51 for legitimate multiple unrelated procedures
- Use -59 for procedures that are usually bundled but were performed separately
Watch Your Global Periods
Many plastic surgery procedures have 90-day global periods (e.g., 19318 – breast reduction, 15847 – abdominoplasty). Any post-op visits or minor revisions within this time are typically not separately reimbursable.
But exceptions exist:
- Unrelated complication management
- New diagnoses
- Different anatomical sites
In these cases, append modifier -24 to E/M services and -78 or -79 to surgical codes.
Cadence Strategy: Use EMR flags to track post-op windows. Automate alerts when claims fall inside global periods, so you can code correctly every time.
Final Thoughts
Medical billing and coding in plastic surgery is anything but routine.
Between insurance complexities, hybrid procedures, documentation nuances, and evolving compliance standards, it’s easy to leave revenue on the table—or worse, face denials and audits.
At Cadence Collaborative, we specialize in helping plastic surgery practices streamline their revenue cycle from end to end.
Whether you’re navigating payer policies for reconstructive care or scaling a self-pay cosmetic program, our team brings deep expertise, hands-on support, and tech-enabled solutions tailored to your practice.
Ready to simplify your billing and boost collections? Book a free consultation with our plastic surgery RCM specialists! Contact us today!